Introduction to the whole process of laboratory nucleic acid detection
Since August, the new crown pneumonia epidemic has once again become the “normal”. Epidemics of varying degrees and scales have appeared around the world, and there are thousands of new crown pneumonia nucleic acid samples waiting for testing every day. How are these samples detected in the laboratory? What does the P3 laboratory look like as the “first battlefield” for humans to fight the new crown virus, and what is the whole process of nucleic acid testing?
According to the level of risk, including the infectivity and harmfulness of infectious pathogens, biological laboratories are divided into four levels: P1, P2, P3, and P4 in the world. The work that can be undertaken by the P1-4 laboratory is also divided according to this safety level, with the strict level from low to high. P3 laboratory, also known as a protection laboratory, is suitable for processing highly hazardous to humans, animals, plants or the environment, through direct contact or aerosols that can infect people with serious or even fatal diseases, or highly harmful to animals, plants and the environment There are usually preventive and therapeutic measures for the pathogenic factors.
How is nucleic acid testing performed in the laboratory?
It can be roughly divided into: pre-test preparations-check sample information-sample inactivation-open the lid and add samples and nucleic acid extraction-PCR reaction system preparation-nucleic acid amplification testing-test completion-autoclave .
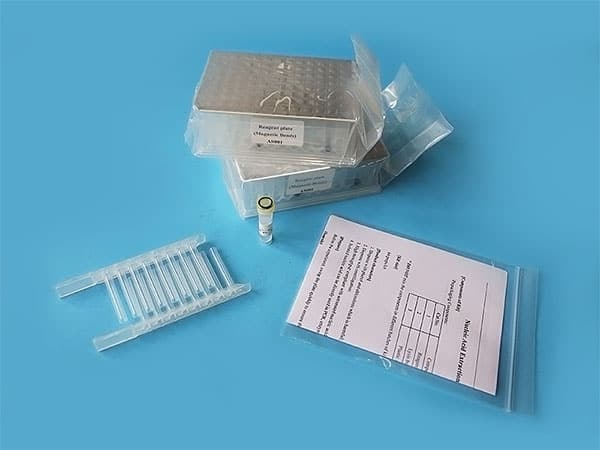
Before testing
Before opening the sample, the inspector needs to wear personal protective equipment, such as protective clothing, masks, goggles, face screens, double-layer medical latex gloves, and waterproof boots. Every step must not go wrong.

Checking
1. Use 75% alcohol to disinfect the outer surface of the sample delivery box in the core area of the laboratory. After disinfection, check the name, age, gender and other information of the tested sample.
2. Put the sample in a water bath for half an hour to inactivate the virus protein at a high temperature of 56℃, so that the virus protein loses its physiological activity, and the virus loses its ability to infect, cause disease and reproduce without affecting the gene sequence of the virus protein. , To ensure the safety of detection.
3. When the experimenter gets the inactivated sample, the first step is to shake, try to let the virus on the swab elute in the medium solution, and the second step is to perform 5 minutes of precipitation. The third part is to open the cover and add samples. This step must be performed manually and requires a high degree of cooperation between two people. One person unscrews the lid of the sample tank, and the other uses a micropipette to suck a small amount of solution in the sample tank, put it in another extraction tube, and then screw on the tube cover.
Nucleic acid extraction can be assisted by instruments, but due to the need for comparison, manual operations are often required, and more than 10 steps such as centrifugation, addition of reagents, and washing are required to be repeated. Among them, there are more than 7 operations that need to open the lid of the tube, and it takes about 50 minutes to complete an artificial nucleic acid extraction.
4. Go out of the core test area, start the PCR reaction system preparation, and add the extracted viral nucleic acid to the nucleic acid amplification detection reagent.
5. Place the prepared PCR reaction on the fluorescent quantitative PCR machine. Set the PCR reaction conditions on the computer, run the instrument, and start nucleic acid amplification detection.

After testing
The tester needs to pay attention to the test situation in real time. After about 1.5 hours, the nucleic acid amplification is completed and the test result is interpreted. At this point, the entire process is completed, about 4 hours.
The last and very important step is to autoclave the contaminants. After the contaminants produced during the experiment are autoclaved, they are treated as ordinary medical waste.
It can be said that the process of nucleic acid detection is also a process of racing against time. Especially in scenarios where large-scale nucleic acid testing is required, transportation to a designated laboratory for testing obviously requires a high time cost. The use of mobile laboratories provides an effective method for improving the efficiency of nucleic acid detection.
For more information about COVID-19 virus nucleic acid testing, please click here:
What is the process of COVID-19 nucleic acid testing?
How to improve the accuracy of COVID-19 nucleic acid testing?



